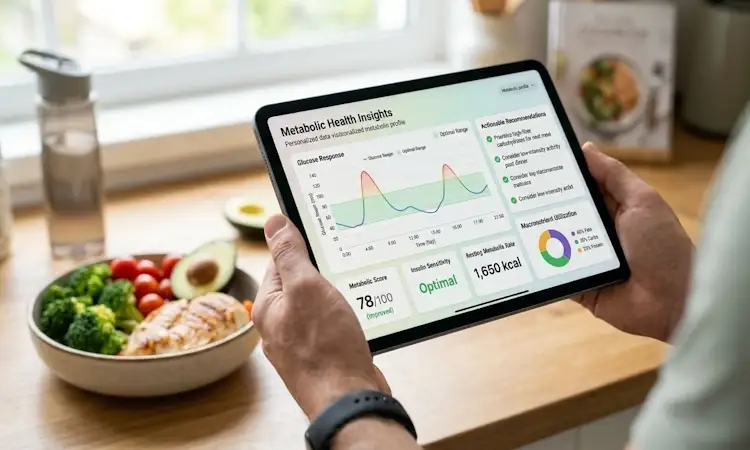
You’ve been doing “everything right.” Meals are planned, workouts are consistent, and you even turned down the office donuts. Still, the scale won’t move, or it drops a pound and snaps right back. After a while, it starts to feel personal, like your body is ignoring the rules.
That frustrating pattern is often called weight loss resistance. In plain language, it means your efforts don’t match your results for long enough that “try harder” stops being useful advice.
Weight Loss Programs
Diet & Weight Loss
Diet & Weight Loss
Diet & Weight Loss
Old School New Body – Transformative Fitness & Nutrition Program
Diet & Weight Loss
This is where metabolic testing can help. It’s not one magic test. It’s a set of tools that measure things like how many calories you burn at rest, how your body stores fat vs muscle, and whether blood sugar or hormones are making fat loss harder. The goal is simple: uncover the likely driver, then adjust your plan with less guesswork. Testing doesn’t replace habits, but it can point you toward the habits that matter most for you.
What weight loss resistance looks like, and why guessing often backfires
A lot of people assume weight loss resistance means they have a “broken metabolism.” Usually, it’s more specific than that. The most common patterns look like this:
You lose weight at first, then hit repeated plateaus that last months. Or you can lose weight only by eating very little, then you regain quickly when you return to normal life. Some people train hard and get stronger, but their waist doesn’t change. Others feel tired all day and hungry at night, even with high “willpower.”
Meanwhile, guessing tends to push you toward extremes. You cut calories again, add more cardio, and tighten rules. That can work short term, but it often backfires by increasing hunger and lowering daily movement. You might also lose muscle, which makes maintenance harder.
It also helps to separate a normal plateau from true resistance. A normal plateau can happen when you’ve lost a few pounds and your smaller body needs fewer calories. Water shifts can hide fat loss for a week or two. A true roadblock lasts longer, even with consistent habits.
Hidden factors are common, and they’re not character flaws:
Portions get underestimated, especially cooking oils, bites, and weekend meals. NEAT (non-exercise activity like steps and fidgeting) often drops without you noticing when you diet. Sleep debt raises cravings and reduces workout quality. High stress makes planning harder and can push you toward “all-or-nothing” eating. Perimenopause can change appetite, sleep, and body composition. Alcohol can quietly add calories and disrupt sleep. Ultra-processed foods can make it easy to eat past fullness. Some medications can increase appetite, cause fluid retention, or change glucose control.
A good metabolic assessment for a weight loss plateau replaces “maybe” with data. That’s why many clinicians use metabolic testing to personalize obesity treatment, as described in this NIH-hosted overview of metabolic testing in behavioral obesity care.
Plateau or resistance, how to tell the difference
A simple checklist can help you decide if you need a deeper look:
- No change for 8 to 12 weeks despite consistent tracking (most days) and a stable plan
- Calories already very low (for example, you’re regularly under 1,300 to 1,500 without medical guidance)
- Strong hunger or low energy that makes adherence feel impossible
- Weight rebounds fast after any increase in food
- Symptoms that suggest a medical factor, like constipation, cold intolerance, hair thinning, or irregular cycles
Talk to a clinician sooner if you have rapid weight change, extreme fatigue, new heart palpitations, fainting, or missed periods.
The “metabolic adaptation” problem after dieting
After weight loss, your body often burns fewer calories than expected for your new size. That’s metabolic adaptation. It’s not sabotage, it’s survival math. Your brain also turns up hunger signals, while you may feel less spontaneous “get up and move” energy.
Aggressive dieting can make this worse. When the deficit is too large, you risk losing more lean mass, your workouts suffer, and your daily movement drops. The obvious response is to cut more food, but that’s like turning down the thermostat when the room is already cold.
Measuring resting metabolic rate (instead of guessing) can show whether you truly need fewer calories, or whether you need a different approach to protect muscle and improve adherence.
The main types of metabolic testing that can uncover a weight loss roadblock
“Metabolism” is a bundle of moving parts. The most useful tests help you answer one question: What’s the main bottleneck right now? In practice, metabolic testing for weight loss usually falls into five buckets.
Here’s a quick map before we go deeper:
| Test or input | What it tells you | Who it helps most | Common limits |
|---|---|---|---|
| Resting metabolic rate (RMR) | Calories burned at rest | Chronic dieters, frequent plateaus | Snapshot, needs proper prep |
| Body composition | Fat vs lean mass changes | Scale not matching effort | Methods vary in precision |
| Glucose and insulin labs | Insulin resistance clues | Cravings, belly weight gain | Needs context and trends |
| Thyroid and related labs | Rule in or out common issues | Symptoms fit thyroid patterns | Not a “routine” fix for everyone |
| Lifestyle screens (sleep, iron, movement) | “Metabolism-like” blockers | Fatigue, low recovery | Requires habit follow-through |
A slow metabolism evaluation for weight management works best when you match the test to your story, not when you order everything “just in case.”
Resting metabolic rate (RMR) testing, how many calories you burn at rest
An RMR test (often done with indirect calorimetry) is basically a guided breathing test. You sit or lie still while a device measures oxygen use and carbon dioxide output. From that, it estimates how many calories your body burns just to keep you alive.
Results usually compare measured RMR to a predicted RMR (based on age, sex, height, and weight). Sometimes the measured number is close. Other times it’s meaningfully lower or higher. That difference can explain why an online calculator feels “wrong.”
Who benefits most?
- People with a long history of dieting and regaining
- Smaller-bodied people who can’t keep cutting calories safely
- Very active people who plateau despite consistent training
- Anyone afraid to eat more because past increases led to gain
Limitations matter. It’s a single day snapshot, so prep counts (no hard workout right before, minimal caffeine, and good sleep when possible). Also, RMR does not include steps, chores, or workouts, so it’s not your full daily burn.
If you want a plain-English breakdown of what RMR means and why it’s measured instead of predicted, see this overview of resting metabolic rate basics.
Advanced body composition testing, why the scale can lie
Two people can weigh the same but have very different bodies. Body composition testing helps you see what the scale can’t: fat mass vs lean mass (muscle, water, organs, bone).
This matters because losing muscle lowers your daily burn and changes how you look and feel. On the other hand, gaining muscle can hide fat loss on the scale. Your jeans might fit better while weight stays the same.
Common methods include:
DEXA scans, which estimate bone, lean mass, and fat distribution. Bioelectrical impedance (BIA), which uses a small electrical signal and can shift with hydration. Skinfold measurements, which can be useful with an experienced tester but vary by technique.
Waist measurements often add clarity, especially when the goal is lower visceral fat risk.
If you’ve been stuck and want practical plateau troubleshooting that includes body composition, this guide on weight loss plateaus and strategies offers helpful context.
Insulin resistance testing for stubborn fat, what to ask for
Insulin resistance is when your body needs more insulin than normal to move glucose from your blood into your cells. Think of insulin as a key and your cells as a lock. With resistance, the key still works, but it takes more force. That higher insulin environment can make hunger worse and fat loss harder for some people.
The most common labs to discuss with your clinician include:
- Fasting glucose
- Hemoglobin A1C (a 2 to 3 month average of blood sugar)
- Fasting insulin (sometimes added to improve the picture)
- In some cases, an oral glucose tolerance test (OGTT)
Clues that insulin resistance testing for stubborn fat may be worth discussing include belly-focused weight gain, intense carb cravings, afternoon energy crashes, PCOS history, or a strong family history of type 2 diabetes.
Don’t self-diagnose from one number. Labs need context, symptoms, and trends. If you want to understand the common testing options before your appointment, this explainer on ways to test for insulin resistance can help you ask better questions.
When thyroid and other labs make sense, and when they do not
Thyroid issues can contribute to weight changes, but they’re often over-blamed. Testing makes the most sense when your symptoms match. Common signs include cold intolerance, constipation, dry skin, hair thinning, heavy fatigue, and feeling “slowed down” even with enough sleep.
Typical labs a clinician may consider include TSH and free T4. In some cases, they’ll add free T3 and thyroid antibodies, especially if autoimmune thyroid disease is a concern.
Other labs sometimes tied to “slow metabolism” feelings include iron (ferritin), B12, and vitamin D. Low iron can make movement feel harder, which reduces daily burn even if your metabolism is fine. Sleep apnea screening can also matter if snoring, morning headaches, or daytime sleepiness show up.
Stress is part of the conversation too. Even if cortisol labs are normal, chronic stress can wreck sleep and raise snack cravings. Those effects are real, even without an abnormal test.
For a research-based look at how thyroid hormones relate to weight and metabolic measures during dieting, see this NIH-hosted paper on thyroid hormones and weight change.
A helpful mindset: tests don’t “prove you can’t lose weight.” They show where your plan needs to get more specific.
How to use your results to build a plan that finally feels doable
Testing only helps if you use the results to set targets you can live with. Start by building your daily calorie needs from two pieces: your resting burn (measured or estimated) and your activity (steps, work demands, workouts). Then pick a deficit that fits your history.
If you’ve been stuck in a cycle of very low calories, you may need a smaller deficit than you think. In some cases, the best next move is eating a bit more while you rebuild training quality and daily movement. That can feel scary, but it’s often the most realistic path to steady fat loss.
Keep the basics tight and boring:
Aim for higher protein to protect lean mass, plus fiber for fullness. Strength train to keep muscle while dieting. Set a step goal you can hit on most days, even when life is messy. Treat sleep like part of the plan, not a bonus.
Personalized metabolism testing for dieting challenges can also highlight when you should shift priorities. If insulin resistance shows up, glucose control habits may reduce hunger first, then fat loss follows. If body composition shows muscle loss, your “plateau” may be a body-rebuild phase.
Work with a registered dietitian or clinician when labs are abnormal, medications may be involved, or there’s any history of disordered eating. Safety comes first.
If your measured metabolism is lower than expected, what to do next
If your RMR is lower than predicted, the fix usually isn’t another aggressive cut. Try these steps for the next month:
- Stop extreme deficits, aim for a moderate calorie target you can repeat
- Raise protein, spread it across meals to support fullness
- Lift weights 2 to 4 times per week, focus on progressive overload
- Increase daily steps, because NEAT often drops during dieting
- Improve sleep consistency, especially wake time and bedtime routine
- Review medications with your clinician, since appetite and fluid changes are common side effects
Small food increases paired with better training can improve energy and reduce binges. The scale may move slower at first, but the plan becomes sustainable.
If insulin resistance shows up, how fat loss strategies change
You don’t need a perfect diet. You need fewer blood sugar swings and more muscle demand. Useful levers tend to be simple:
Consistent meal timing helps many people. A protein-focused breakfast often lowers cravings later. High-fiber carbs (beans, oats, berries, potatoes with skin) usually work better than low-fiber sweets. Cutting sugary drinks is a quick win. Strength training improves insulin sensitivity, and so do short walks after meals.
Progress may show up first as less hunger, fewer crashes, and a smaller waist, even before big scale changes. If PCOS or prediabetes is part of the picture, discuss medical options with your clinician.
Conclusion
Weight loss resistance is common, and it’s rarely about effort. The real issue is usually a mismatch between the plan and your physiology, your lifestyle, or both. The right tests can clarify whether your roadblock is low resting burn, changes in body composition, insulin resistance, thyroid problems, medication effects, or “metabolism-like” factors such as sleep apnea, low iron, or low daily movement.
No single test is magic. Still, a targeted workup can prevent months of trial and error, and it can make your next steps feel simpler.
Write down your symptoms, dieting history, and typical week. Then ask your clinician which tests fit that story. Finally, use the results to choose one or two focused changes for the next four weeks, because consistency beats intensity when you’re trying to unstick progress.

The content provided on tokeepyoufit.com is intended for general informational and educational purposes only. All materials on this site, including articles, recipes, tips, guides, opinions, and product recommendations, are not a substitute for professional advice from a qualified medical, nutrition, or fitness expert. Users should consult a licensed professional before making any decisions related to health, diet, or exercise. Please read our full Medical Disclaimer here.
Dietary Supplements
Dietary Supplements
Dietary Supplements
Nagano Tonic – Daily Support for Energy, Vitality, and Balance
Dietary Supplements
Neuro-Thrive – Daily Brain Support for Focus and Cognitive Clarity
Dietary Supplements
ZenCortex – Daily Support for Brain Clarity and Hearing Health